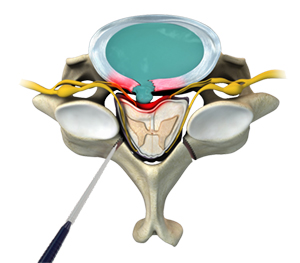
What is Minimally Invasive Ultrasonic Laminectomy?
Minimally invasive ultrasonic laminectomy is a surgical procedure that uses advanced ultrasonic technology to remove a portion of the vertebral bone (lamina) to relieve pressure on the spinal cord or nerves in a precise and tissue-sparing manner. This technique is part of the broader field of minimally invasive spine surgery (MISS) and is typically used to decompress spinal nerves and relieve symptoms caused by compressive spinal pathologies.
What are the Indications for Minimally Invasive Ultrasonic Laminectomy?
Minimally invasive ultrasonic laminectomy is commonly indicated to treat spinal conditions, such as spinal stenosis, herniated discs, facet joint hypertrophy, degenerative spine conditions, or bone spurs that compress nerves in the lumbar spine.
What Does the Procedure for Minimally Invasive Ultrasonic Laminectomy Involve?
The procedure for minimally invasive ultrasonic laminectomy involves using a specialized ultrasonic device to precisely remove part of the lamina (the back part of the vertebra) to decompress spinal nerves, all through a small incision with minimal disruption to surrounding tissues.
In general, the procedure involves the following steps:
- The patient is given general anesthesia and positioned face down (prone) on a specialized surgical table to expose the spine.
- A small (typically less than 2 cm) incision is made over the affected vertebral level. A tubular retractor is inserted to create a working channel down to the spine, gently pushing aside muscles instead of cutting them.
- A surgical microscope or endoscope is inserted through the retractor to provide high-definition, magnified views of the surgical area.
- A high-frequency ultrasonic bone scalpel is used to selectively remove the lamina. The ultrasonic device precisely cuts bone while sparing adjacent soft tissues like the spinal cord, nerves, and blood vessels.
- Additional bone (such as part of the facet joint or ligamentum flavum) may be removed to fully decompress the spinal canal and relieve pressure on the nerves.
- Once decompression is complete, instruments are removed, and the incision is closed with a few sutures or surgical glue. A small bandage is applied.
What Does Postoperative Care for Minimally Invasive Ultrasonic Laminectomy Involve?
Following the surgery, patients are typically monitored for a few hours or overnight and can often go home the same day or within 24 hours. Pain is usually mild to moderate and managed with oral medications. Walking is encouraged soon after surgery to prevent stiffness and improve circulation. Patients are advised to avoid heavy lifting, twisting, or bending for several weeks. Follow-up visits are scheduled to monitor recovery, and physical therapy may be recommended to strengthen the back and improve flexibility. Most individuals can return to light activities within a few days and resume normal routines within a few weeks, depending on the complexity of the procedure and individual healing.
What are the Risks and Complications of Minimally Invasive Ultrasonic Laminectomy?
Risks and complications associated with minimally invasive ultrasonic laminectomy include the following:
- Nerve injury (though less likely with ultrasonic tools)
- Dural tear (cerebrospinal fluid leak)
- Infection or bleeding
- Incomplete decompression
- Spinal instability
- Recurrence of symptoms in some cases
What are the Benefits of Minimally Invasive Ultrasonic Laminectomy?
The benefits of minimally invasive ultrasonic laminectomy include the following:
- Reduced postoperative pain
- Faster recovery
- Minimal blood loss
- Smaller scar
- Reduced muscle and tissue damage
- Lower risk of nerve injury and spinal instability





